 Peak flow meters are an important tool in your kit bag to measure the volume and effectiveness of somebody’s lung capacity and the way they are breathing. It is most commonly used with patients with specific lung conditions such as bronchitis or emphysema. People who have COPD, Chronic Obstructive Pulmonary Disease, also use it. COPD is a reduction in the surface area of the lungs, reducing their efficiency. Peak flow calculations are also used when assessing a patient with Asthma.
Peak flow meters are an important tool in your kit bag to measure the volume and effectiveness of somebody’s lung capacity and the way they are breathing. It is most commonly used with patients with specific lung conditions such as bronchitis or emphysema. People who have COPD, Chronic Obstructive Pulmonary Disease, also use it. COPD is a reduction in the surface area of the lungs, reducing their efficiency. Peak flow calculations are also used when assessing a patient with Asthma.
The Peak Flow Meter
The meter itself has a mouthpiece where the air enters the airway measuring system. There’s a scale on the outside which measures the amount of air that is blown into the unit itself. It also has two different types of mouthpieces. The most commonly used is the one-use cardboard tube that is disposable. The other is a clean, sterile, reusable mouthpiece. These tend to be used less due to contamination.
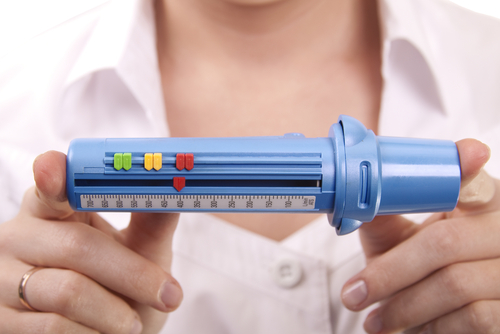
The cardboard mouthpiece pushes into the end of the peak flow meter. The patient must make a seal around the cardboard tube with their mouth. The patient’s tongue and teeth need to be clear of the actual inlet valve for this to work effectively, so tell them not to do this. They need to take as deep a breath as they can, and, in one short blow, blow into the meter. The needle and scale will raise to give you a measure of the capacity and the force the air that has left the lungs. This must be repeated three times, and use the highest of the three tests. This gives you the level and capacity of the lungs of the patient. This helps to give a baseline set of observations to tell you how effective treatment is.
Using the Peak Flow Meter
Once you have administered drugs or nebulisation, their lung capacity should improve. The only way we can find that out is by taking an initial reading before giving the drugs. Once the drugs get into the system, wait a short while and repeat the measurement again. There should be an improvement in the capacity of the lungs. This gives you some idea if the treatment is working and can be evidenced on the patients’ report forms. It is advised to do the three blows before but it is not absolutely crucial. If you encounter a patient that has a very severe breathing problem, do not waste time taking peak flow readings. Write on your patients report form that the patient was too ill or the breathing was too bad to perform a peak flow reading.
For more information on training courses, visit our “Courses” page which also includes our First Responder and First Person on Scene (FPOS) Courses.


Pingback: Basic airway management to maintain a patients breathing